What is Ectropion?
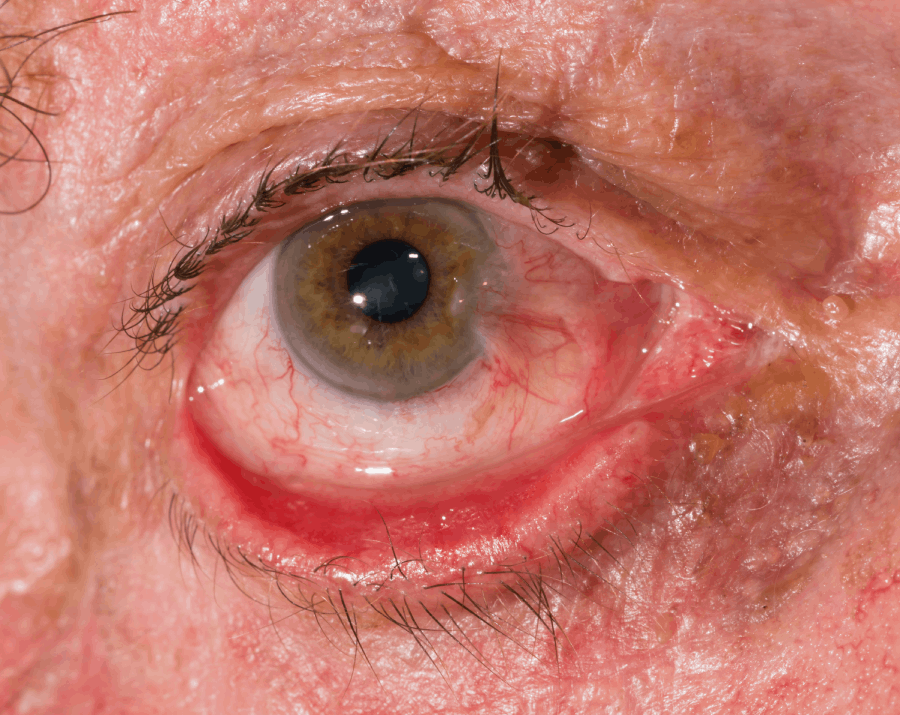
Ectropion is a common condition where the eyelid sags and with the eyelid margin turning outwards, away from the eye. Ectropion can irritate the eyes and lead to repeated eye infections and, in severe cases, corneal ulcers. Ectropion is one of the most common eyelid procedures, with surgical ectropion repair having a high success rate.

Types & Causes of Ectropion
The most common cause of ectropion is due to age-related changes to the structural support of the eyelids. This type of ectropion is called Involutional Ectropion, which usually occurs from around the age of 60 onwards. As you age, your facial muscles weaken and sag, which particularly affects the lower eyelid since the muscles surrounding the tendons and ligaments become lax.

Hover on image to see ectropion example
However, there are several other different types of ectropion to be aware of that are caused differently.
- Cicatricial Ectropion: caused by skin scarring, which pulls the eyelid outwards. Burns, trauma, previous eyelid surgery and skin conditions, including rosacea, can all have this effect.
- Paralytic Ectropion: caused by facial paralysis damage to the innervation of the muscles that supply the eyelid, usually seen following Bell’s palsy, facial nerve palsy.
- Mechanical Ectropion: caused by the weight of a mass pulling the lower eyelid down and outwards.
- Congenital Ectropion: caused when the lower lid margin has been turned outwards since birth and is the rarest type of ectropion.
- Ectropion after blepharoplasty. This is a very complex problem to treat and can be due to all the above causes. Please see the revision blepharoplasty page for more details on how this can be approached.
Complications of Ectropion
Once you've developed an ectropion, the structural changes to the eyelid muscles that cause it are unlikely to be resolved without surgery. In most cases, your symptoms may slowly progress. However, repeated infections are common, and in severe cases, corneal infection or ulceration may develop.
SYMPTOMS & SIGNS OF ECTROPION
Symptoms
Ectropion has multiple symptoms you may experience, so it’s essential to ensure you are attentive to how severe they can become.
- Watery Eyes: As the eyelid moves away from the eye, it prevents tears from draining correctly into the puncta, causing tears to pool and constantly flow over the edge of the eyelid onto the cheek.
- Ocular Irritation: Due to the exposure of the conjunctiva, which normally resides next to the eyeball, it can become very sore.
- Mucoid discharge: Creamy discharge is common due to ocular irritation and lack of tear drainage.
- Redness: Exposure of the conjunctiva gives the appearance of a very red lower eyelid.
- Sensitivity to light and wind: Irritation to the cornea's surface causes increasing sensitivity to light and wind.
Signs
You should seek immediate medical advice if you see any of the following signs, as they may indicate the development of an eye infection or corneal ulcer.
- The white of your eye has become very red.
- Your sensitivity to light and wind is quite strong.
- Any change in your vision.
- Copious discharge.
- Pain
- If you see a white spot on the cornea
Note: Ectropion may be diagnosed by an optician or GP who can refer you to an ophthalmologist for further assessment and treatment.
Tips to Improve Symptoms
Correcting the problem without surgery is impossible, but improving the symptoms with simple steps is possible.
For example, using eye lubricants such as artificial tears can maintain ocular surface wetting, prevent vision-threatening damage, and improve discomfort. If the lower eyelid skin has become dry and cracked, this can be treated with simple eczema treatments like emollient cream. The lower lid can be massaged upward to counter the downward contraction in the skin.
ECTROPION VS ENTROPION
Both Ectropion and Entropion are conditions that affect your eyelid and are typically more common among older individuals. The eyelid conditions also cause similar symptoms, such as redness and watering of the eyes.
Differences:
- Ectropion is when your eyelid turns out and doesn’t touch your eye.
- Entropion is where your eyelid turns in and then results in your eyelashes to rub against the cornea, irritating the eye.
DIAGNOSIS OF ECTROPION
Ectropion can be diagnosed by an optician or GP who can refer you to an ophthalmologist for further assessment and treatment.
If you have Ectropion, it can be diagnosed with a routine eye exam. You can expect your doctor to ask you to close your eyes and check your eyelids to assess the eyelid muscles and their tone and tightness.
Also, if you have any scars, tumours or have had a previous surgery, it is good to provide medical history for your doctor to give a thorough assessment.
At Ezra Clinic, you can expect to get a highly experienced consultant from our team to do an extensive examination and find the right treatment for you and your symptoms. Don’t leave your symptoms untreated.

Ectropion Surgery Overview

Undergoing the ectropion surgery is the only treatment option that can permanently correct the eyelid position.
Once diagnosed your ophthalmologist will discuss your medication with you, and you may be asked to stop taking some medication prior to surgery. Therefore, it is important to tell your doctor if you take any specific medication due to any possible side effects or reactions.
The procedure you receive and the time it takes to perform it will vary depending on your ectropion type. Depending to the type you have, the general time to complete the ectropion treatment is 30 to 90 minutes.
Note: You may spend around half a day in our clinic when allowing for preparation and aftercare.
Preparation for Surgery
Depending on your planned anaesthesia, your doctor will advise you when to stop eating or drinking but the ectropion treatment usually only requires local anaesthesia with intravenous sedation, ensuring you are comfortable and sleepy throughout the procedure.
During the Surgery
The general, age-related (involutional) ectropion surgery involves tightening the lower eyelid with stitches on the outside corner of the eye. Nevertheless, depending on the type of ectropion you’re diagnosed with, the procedure will require a specific technique during the surgery.
- Cicatricial ectropion may require a skin graft or flap in addition to the lower lid tightening of the eyelid. The skin may be taken from the upper eyelid, in front or behind the ear or from the upper arm. The exact spot will be based on several patient factors, including skin excess, colour, and texture.
- Mechanical ectropion depends on managing the eyelid lesion and usually involves a biopsy followed by further surgery.
- Paralytic ectropion: A comprehensive approach must be taken in association with facial weakness to protect the eye's surface and prevent visual loss.
During the procedure, we also aim to minimise any significant scarring by making incisions along the eyelids' natural creases. Stitches are usually removed at one to two weeks.

Post-Surgery Aftercare
For most patients, the surgery will correct ectropion almost immediately.
Like with any surgical procedures, there may be some short-term discomfort. As well as, experiencing some bruising and swelling around the area that has been operated on after surgery, but it will usually subside between one and two weeks.
After the procedure, patients will be advised to:
- Use antibiotic ointment on the area for one week
- Use cold compresses to reduce bruising and swelling
Consider that post-surgical complications such as bleeding or infections are uncommon but are a risk after any operation. Following the aftercare advice is essential so the eyelid can heal properly.
If you are experiencing any ectropion symptoms or signs, don’t wait and request a consultation with us now.