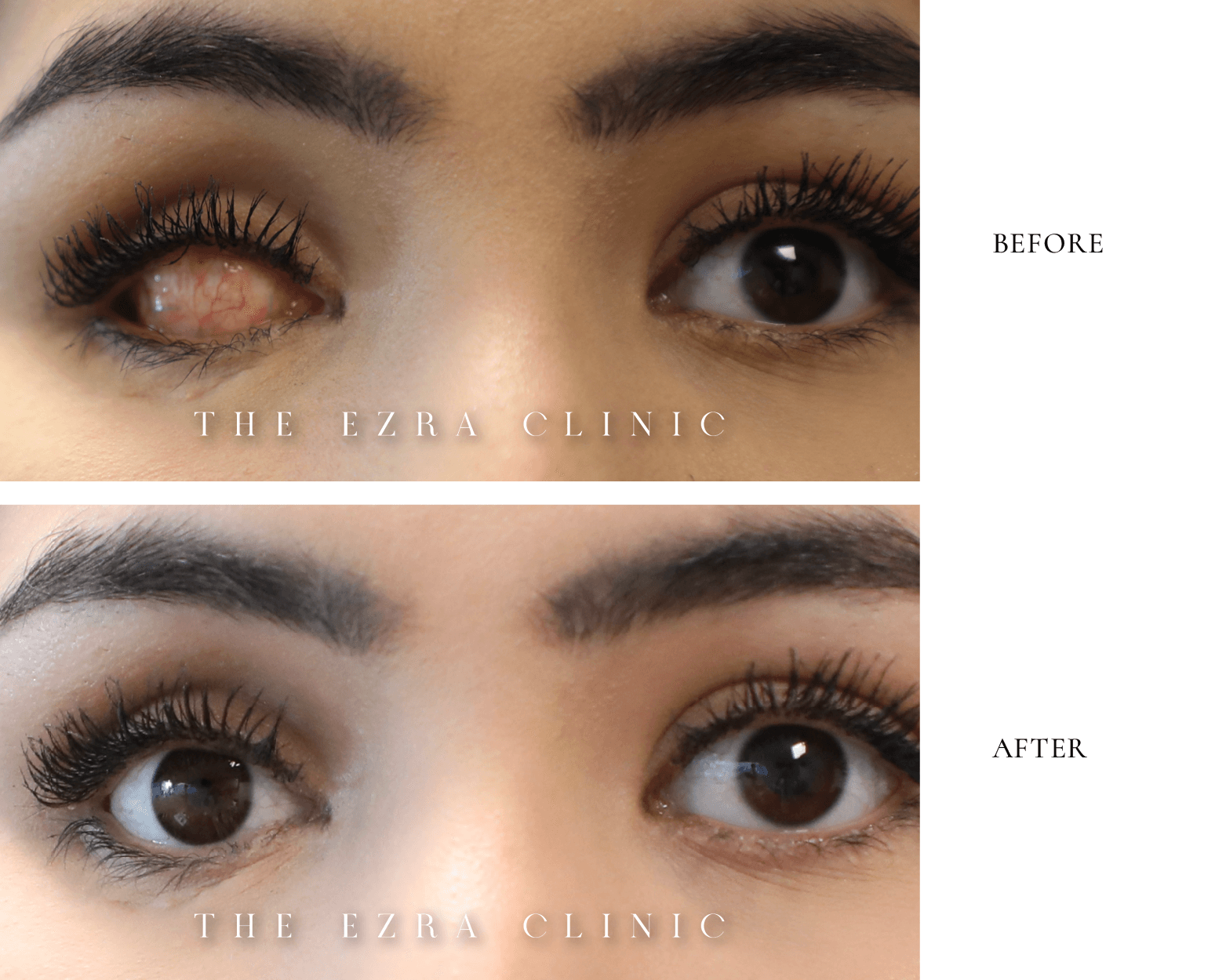
Aftercare – What Is the Recovery Process Like?
It is important to be ready for a relatively lengthy aftercare process after prosthetic eye surgery. This is a significant and impactful procedure that can lead to some side effects.
When the surgery ends, the surgeon will apply a dressing to cover the area, which should be removed about 24 hours post-operation. The transparent shell fitted during surgery will be visible. This shell has a hole in the middle to assist with drainage and airflow and to allow medications to be administered. You must keep this in your eye socket until it has healed and can tolerate a custom eye being fitted.
The area around the eye and the eyelids may exhibit redness, swelling, bruising, and sensitivity, which will gradually improve over time, with the redness fading to pink. It is normal to experience pain and soreness in the eye for a few days, as well as headaches, which can be treated with painkillers. Nausea is another possible side effect.
You will also likely be prescribed eye drops, ointment, or both to apply several times a day to clean the eye and minimise the risks of infection. Antibiotic treatment and pain medication may also be prescribed. It is best to keep the eye uncovered as much as possible to encourage airflow and healing, though wearing dark glasses occasionally for comfort is acceptable.
Finally, your specialist will schedule a follow-up appointment to assess how the eye is healing and discuss the next steps in the process.